Sometimes I forget.
Forget why we began this trip, this new RV life. How easy it is to get caught up in the middle of life — with all its ups and downs — and forget how far we’ve come.
But when I revisit pictures like this, I am reminded of how far we’ve come together as a family, in regards to our health, and how much we love each other.
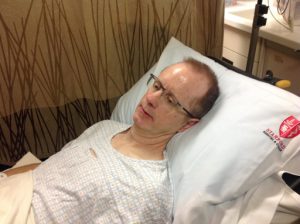


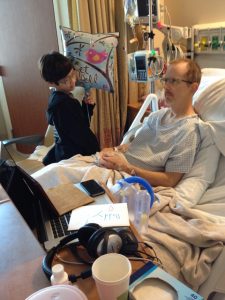

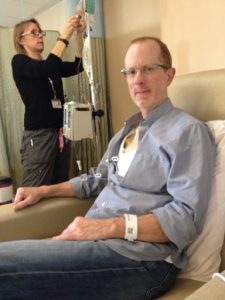

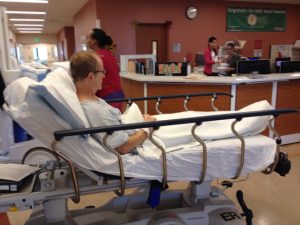





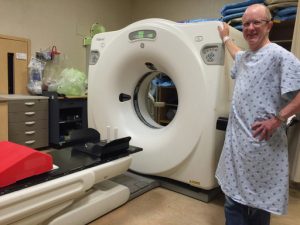



These pictures were taken between 2014 and 2015, when my husband of almost 22 years, Darrell, [if interested, he has his own separate blog] was diagnosed with cancer, when we dreamed up the idea to reduce overall stress in our lives by quitting our traditional 9-5 jobs, stop paying for a mortgage for a SF Bay Area house we could barely afford, and live and travel the world together in a RV as a family.
There’s still some stress now, but it mostly stems from work-related and time-management stress as we both work on-the-road part-time chasing wi-fi.
But nowhere near the stress of worrying that you don’t have much time on this earth with the love of your life and your son and stepdaughter’s father, burdened with high costs and massive amounts of debt.
In 2014, when Darrell went into his regular General Practitioner’s for a cough that refused to disappear, he discovered something was amiss when the chest x-ray technician gasped at the sheer size of the mass that appeared on his black and white screen. From there, it became a mystery game, a hunt to discover if he even had cancer, and if so, what kind.
Most importantly, we all wanted to know: How long did he have left to live?
We were at a loss as to what to do. Should Darrell turn vegetarian again? He had been vegetarian for over 15 years. I imagined the freezer full of Morningstar burgers and fake bacon. I had recently adopted a Paleo diet and it had already helped me come off all my meds, but I still had weight to lose. Other friends suggested juicing and the Gerson Therapy. Others suggested other alternative therapies. We didn’t know what to do, what to choose.
Only three years before, Steve Jobs had died and I read up on all kinds of diets and scenerios, imagining the worst outcomes possible. But then a good friend who followed a Paleo/Primal way of eating Darrell’s mentioned the ketogenic diet. “There’s talk that cancer feeds on sugar, on glucose,” he informed us while visiting from out of state.
A former biology/chemistry major, Darrell immediately latched onto the science and chemistry behind the ketogenic diet. It made sense. We began searching online and came across Ellen Davis, Dominic D’Agostino, and Miriam Kalamian. I immediately bought e-books and devoured everything I could on the subject. My sister, who had lovingly spent much of her time babysitting and helping me with my virtual assistant clients while we went to doctor appointments and during hospital stays for the two biopsies, introduced me to the audio book by Jimmy Moore: Keto Clarity. Later, I found Patricia Daly, Martina Slajerova, as well as Maria Emmerich.
In the meantime, as I learned how to cook and eat keto, I adapted many of the Paleo recipes I had from all the Paleo cookbooks I had amassed, such as Melissa Joulwan and Michelle Tam of Nom Nom Paleo. I encouraged Darrell to reach out to Miriam Kalamian for a Skype consultation, and he did. She was extremely helpful and encouraging, and I remember making my first mug cakes from recipes she had sent us, in addition to the ones I was making out of her e-book.
At first we didn’t know what type of cancer Darrell had. It was right before Thanksgiving in 2014, and Darrell’s fantastic oncologist in (Alta Bates Summit) Berkeley pulled some strings and found a doctor who would do a biopsy in Concord, at John Muir Hospital. That doctor speculated Darrell might have thymoma. Then there was talk among other doctors brought in that it could be a teratoma. We looked it up. Could Darrell’s tumor have teeth, have hair? Even through the despair, we found a moment to joke around. What if Darrell had a miniature clone growing inside his chest, where the tumor was located? That year, we skipped Thanksgiving, spending it in the hospital.
We were told Darrell needed to stay in the hospital for several days. He was fed orange juice, sandwiches, dessert. While Darrell had the biopsy which would take quite some time, per the doctor, my sister, my kid and I sat in the waiting room, taking turns playing the piano. We also spent some time in the chapel area, writing heartfelt notes, wishing and praying for the best possible outcome. The doctor at John Muir pulled me aside after the biopsy was over to inform me that he believed Darrell had a thymoma that would require open-heart surgery, chemo, and radiation. “He’s not going to be able to work anymore, not for some time. In fact, it will be hard,” he said gruffly, a doctor with not the best of bedside manners. And with that he was gone. I was left in tears, worried about my husband’s chest cut open, the danger around cutting near the aorta. Later, I remember being comforted by my sister-in-law over the phone shortly after.
No one ever tells you how time seems to slow down when you’re awaiting a cancer diagnosis. Especially around the holidays.
After about a week, the biopsy came back: Inconclusive. The doctor had cut around Darrell’s chest area and there still wasn’t an answer?? We were disappointed and angry. So was Darrell’s oncologist. Apparently, he chewed out this doctor at John Muir who had recommended we go ahead and act as if this were a thymoma. Again, Darrell’s oncologist pulled some strings, and this time, sent him to Stanford, even though it was now close to Christmas. We were worried time was running out. Would we have time to shrink the seemingly unusually large tumor?
Our answers came easily at Stanford. This time, the doctor we were assigned to who did the biopsy was easygoing and made us feel at ease immediately, unlike the one at John Muir. He guessed it was lymphoma, not thymoma, and he was right. The biopsy was quick and easy, a short outpatient visit, and within a day or two, we found out Darrell was diagnosed with Hodgkin’s Lymphoma (Stage 2B). The doctor assured us that if there was a cancer to get, this was “a good one.” Again, we laughed. Relieved. But our oncologist was still concerned with the size of the three tumors (7, 3, and 2 cm). He had three near his heart, and the chemo would have to pass through his aorta. I worried about how fragile that area was, how fragile the heart can be. Would he be able to handle it? (A lesson learned here: Just because someone is an esteemed rock-star doctor, he may not know all the answers. You are your own best advocate when it comes to your own health. Don’t be afraid to get a second opinion.)
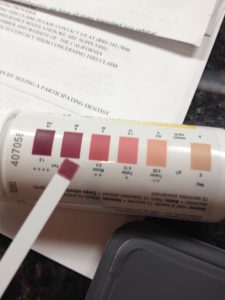
But at the same time, we were both ramping up the ketogenic diet, now following Miriam Kalamian’s advice in her book, along with other keto for cancer books out at that time in 2015. We bought a scale, Ketostix at first, used MyFitnessPal for macros, then the Precision Xtra to measure glucose and ketones, discovering Dr. Thomas N. Seyfried’s book that Darrell immediately downloaded onto his Kindle, a dense medical book that recommended that the GKI be as close to 1 as possible. I wrote a blog post for Heads Up Health, a client of mine, about how Darrell and I tracked his Glucose Ketones Index during his cancer, and still do, now in remission. He included some fasting as well. To support Darrell, I decided to eat mostly keto too. I was also intrigued to see if it could help my moods as someone once diagnosed with Bipolar Type II, having read in Keto Clarity that the keto diet had the potential to help those suffering with this disorder. I had been off all meds–including asthma–simply reducing the amount of flour and sugar back in 2012, and was encouraged by what a Paleo/Primal diet could do. Also, my doctor had warned me that with my latest HBA1C, I was now diagnosed with prediabetes. (In 2016, we began tracking our health using Heads Up Health, enjoying the ability to import medical records from different labs and using the Analyzer graphing feature to see how far we’ve both come in terms of our health, motivating us to continue staying keto-adapted.)
The oncologist, radiologist and the nurses in the chemo infusion room all noticed how rapidly Darrell’s tumors were shrinking. They also remarked on Darrell’s lack of the usual symptoms post-chemo: no hair loss, no nausea. Even though all food Darrell ate tasted like metal, he enjoyed eating the mug cakes, the fat bombs, bone broth and all the keto food I made using a Paleo/Primal lens. We kept his net carbs really low, at 12 net carbs, weighing and measuring portions, afraid to eat too much protein then, due to gluconeogenesis. I pricked my finger alongside Darrell daily, checking our blood glucose and blood ketones (beta-hydroxybutrate/BHB), then making sure his GKI was low as possible. The fasts helped with the chemo, lowering insulin and raising ketones. “Whatever you’re doing, keep doing it!” One nurse smiled warmly at us after checking Darrell’s blood test results before beginning his hours-long infusion, seated in a lazy-boy-like recliner, his laptop still propped on his lap as he refused to quit working full-time. His employers were understanding, wanting him to take time off, but working gave Darrell something else to think about, and this was what he wanted then.
During this time — several months — of weekly chemo infusions, Darrell stopped taking the BART train for fear of catching colds, compromising his immune system. Instead, he took a commuter bus near Oakland that brought him into San Francisco where he worked downtown for a FinTech company.
Although I know the treatment and oncologist helped, what Darrell and I both know today is that eating keto played a part in quality of life, and we feel it in our bones that it also helped in the rapid shrinking of the large tumors that resided in his chest.



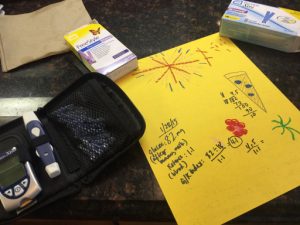



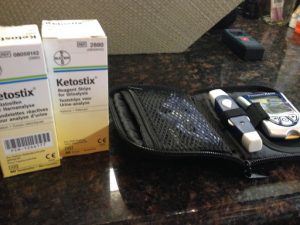
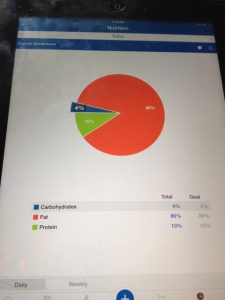




Now it’s 2018 and in October, Darrell will have been in remission for three years. Even though much older now, we are both now in the best shape of our lives. Although not 100% compliant every single meal, we still incorporate keto eating and fasting into about 90% of our lives. What keeps us keto-adapted and in ketosis most of the time is tracking our health (e.g., blood ketones, blood glucose) with the Keto-Mojo (much more affordable blood ketone strips than Precision Xtra) and Heads Up Health (e.g., GKI, waist and hip measurements, weight, lab tests like the Hba1c), MCT oil, butter and ghee. And now almost three months in, we’re about to embark on a trip around the world in our RV, finally having the energy to exercise, to pursue our dreams. We recently sold our house in the SF Bay Area and downsized in the biggest way, leaving a 3K+ sq ft house for a 100 sq ft expedition vehicle/RV.





















Life can still be stressful at times, but we have so much to look forward to now.
And with that, I cannot be more grateful.
9 Comments
Leslie · July 27, 2018 at 5:29 am
Jane, wonderful, life-affirming post. Having taking time out at Berkeley to take care of my dear grandmother who was having chemo for a brain tumour, I can relate. When you described Darrell eating orange juice and sandwiches in hospital, I cringed: my grandmother would eat frosted cakes and cookies as an emotional eating coping mechanism. If only we had known about keto then, perhaps the outcome would have been different. Thanks you for spreading the word on keto – all patients should be entitled to know about it.
lily · December 4, 2019 at 4:36 am
Oh Leslie, thank you for your comment and sharing your story. I’m sorry about your grandmother. And also sorry I’m just now seeing your comment to my post about Darrell using keto for cancer in 2014. I think it’s a powerful tool to use food as medicine, in addition to conventional treatment. Wish the hospital nutrition would get up to speed on serving healthier foods to their patients!
waterfallmagazine.com · July 7, 2020 at 10:44 am
https://waterfallmagazine.com
Hi are using WordPress for your site platform? I’m new to the
blog world but I’m trying to get started and create my own. Do you
need any coding expertise to make your own blog? Any help
would be really appreciated!
lily · February 14, 2021 at 7:38 pm
Hi Jeanna, I’m sorry I’m just seeing your message now. I am using WordPress, but don’t know any coding. I look forward to checking out your blog!
Reflections on One Year Living Full-Time in our LMTV / Bliss Mobil RV - Bliss Or Die · March 17, 2019 at 10:08 pm
[…] to conventional cancer treatment. We continue to adhere to keto as much as we can. Check out Lily’s great article on our keto […]
Getting Out of My Comfort Zone | Hellbent On Bliss · December 2, 2019 at 7:05 am
[…] keto as an adjunct to conventional chemo and radiation when my husband got cancer in […]
Days 4 and 5 of a 7-Day Water Only Fast | Hellbent On Bliss · February 1, 2020 at 6:53 am
[…] for more info on the ketogenic diet as it pertains to cancer; and since this is a topic that hits me personally, I felt blessed to be able to help others find info I’d give to my own loved ones–in […]
Self Experimenting is the Key to Building New Habits | Hellbent On Bliss · February 18, 2020 at 3:46 pm
[…] came about when my husband found out he had cancer at the end of 2014. That’s when we began using keto and fasting to help shrink his tumors, along with the chemo and radiation he was doing. I had begun to notice the connection between food […]
The Next Best Thing to Bottling Up Bliss and Ease: Ketosis - Hellbent On Bliss · September 3, 2023 at 7:38 pm
[…] you’re in ketosis; when my husband had cancer in 2014 , now in remission, and we used a therapeutic keto diet as an adjunct with conventional treatment, we aimed to get his GKI under 2 much of the time, after […]